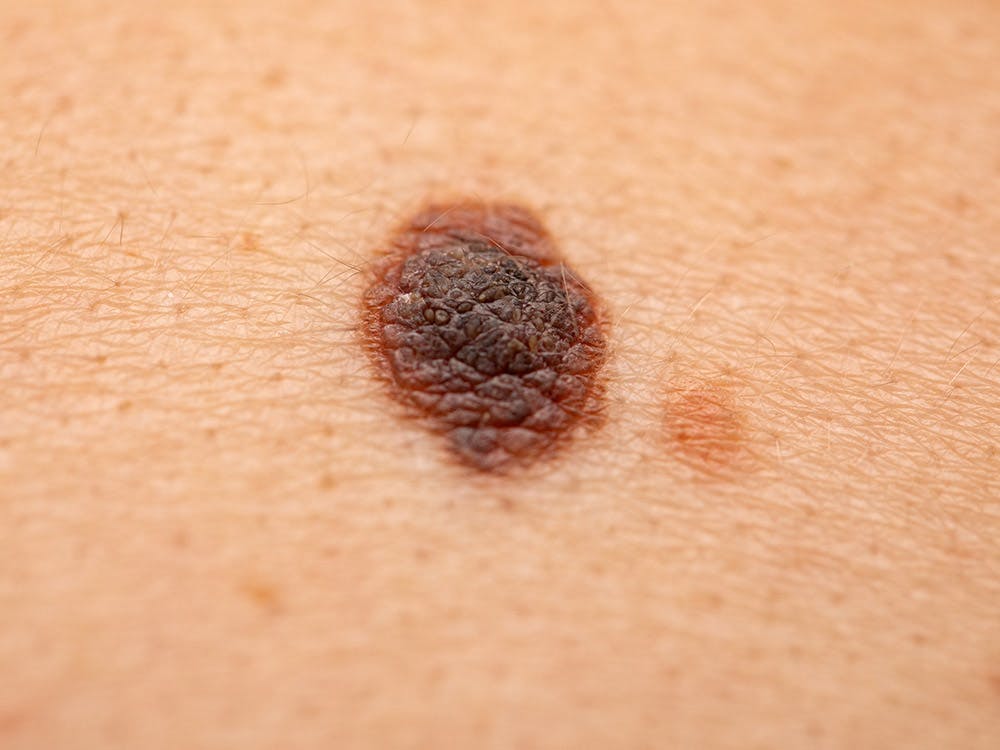
What is melanoma?
Malignant Melanoma (MM) is a highly severe form of skin cancer originating from melanocytes, the pigmented cells responsible for producing melanin in the skin. Melanoma can occur anywhere on the body, including both sun-exposed and non-sun-exposed areas.
Schedule a complimentary consultation today!
ScheduleIs melanoma dangerous?
Melanoma is the most dangerous type of skin cancer because it's more likely to spread and spread to other parts of the body. It's important to get treatment as soon as possible because it can get into other tissues and spread. The type of melanoma you get depends on how advanced it is. If you get diagnosed with stage I, you're more likely to live for a while without having to worry about it coming back. But if you get stage II-IV, you're at a higher risk of getting something worse.
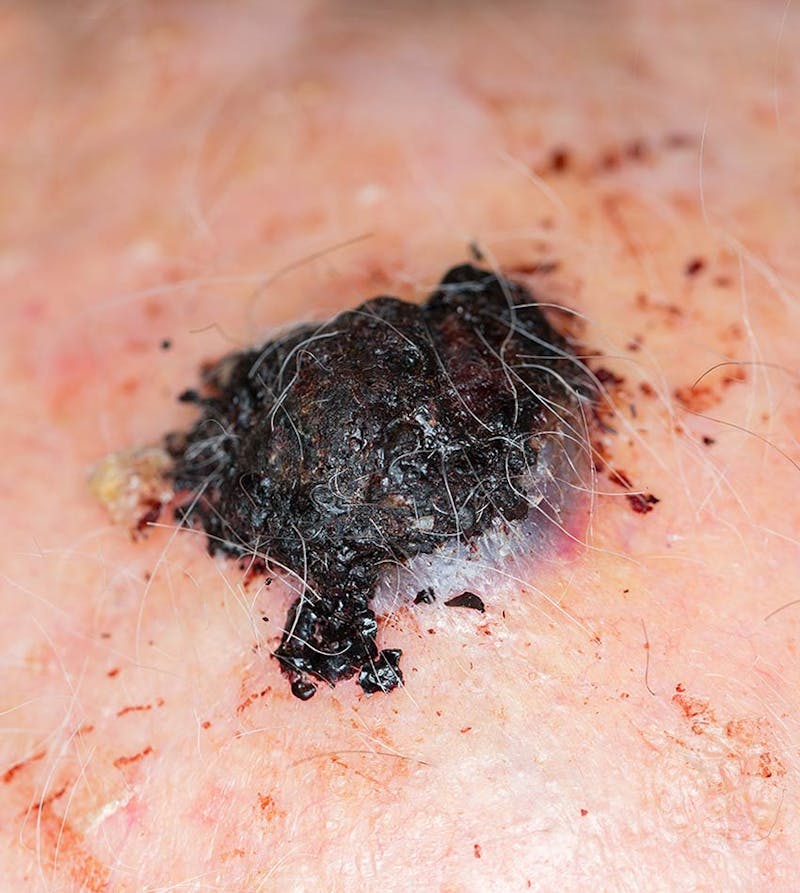
What causes melanoma?
Melanomas develop from the melanocytes that are normally present in the skin’s cell layer of the body. These cells normally function to produce melanin, which gives the pigmentation seen on the skin surface. Melanoma is the result of the abnormal growth of melanocytes developing on the skin surface.
There are different risk factures associated with the development of melanomas, some of which are:
- Skin pigmentation - those with light skin pigmentation are more prone to develop melanomas.
- Nevi or moles - individuals with a large number of moles or atypical nevi have a higher chance of developing melanomas.
- Genetic predisposition - those with a strong family history of melanomas can develop melanomas themselves.
- UV light or sun exposure - unlike non-melanoma skin cancers, which are associated with cumulative sun exposure and tend to form in areas of frequent sun exposure, high intensity and intermittent exposure to the sun’s UV rays, such as sunburns, are associated with melanomas.
What do melanomas look like
Melanomas typically exhibit characteristics resembling pigmented spots or moles. To assess whether these lesions require further evaluation by a healthcare professional, the ABCDEs of melanoma are utilized. These initial features help determine potential concerns:
A: Asymmetrical shape.
B: Irregular borders.
C: Multiple colors within the lesion.
D: Diameter exceeding 6 mm (about the size of a pencil eraser).
E: Evolution, indicating changes in shape, borders, colour, or diameter.
These guidelines serve as general indicators when evaluating melanomas. If you have any concerns regarding a lesion, it is always recommended to seek evaluation from a healthcare professional.

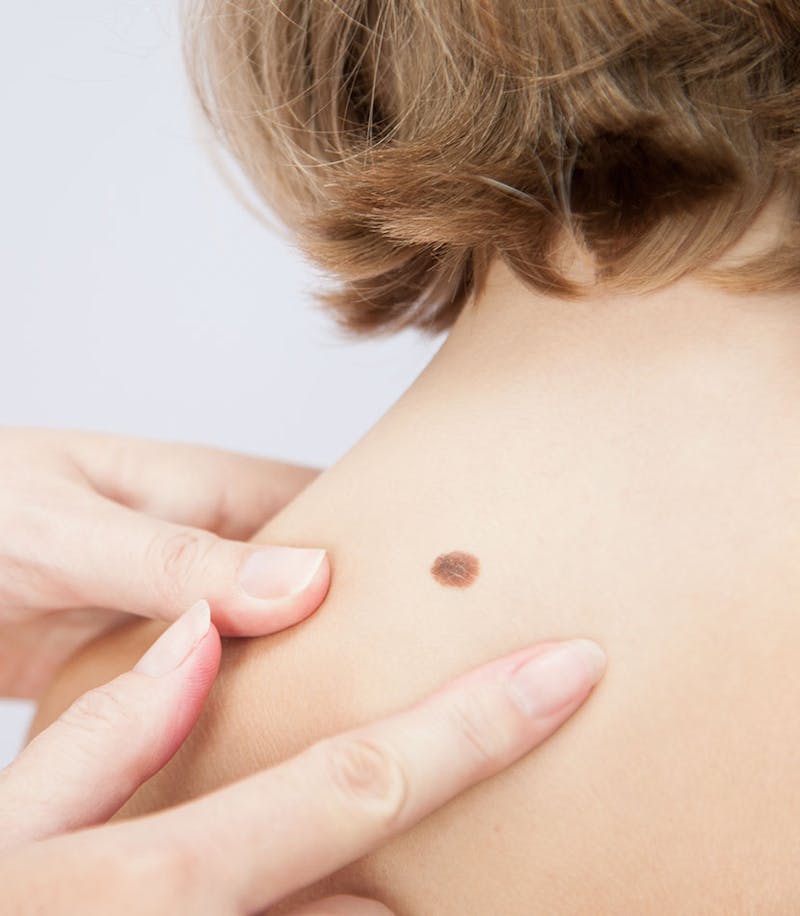
What is the treatment for melanomas?
The treatment approach for melanomas depends on the depth of invasion and the stage of the melanoma after surgical removal of the lesion. When a suspicious lesion is present, a healthcare professional will perform either a punch biopsy or an excisional biopsy to obtain a small sample for diagnostic purposes.
The biopsy sample is then examined under a microscope by a pathologist who determines whether the lesion is a melanoma and assesses its depth of invasion. The depth of invasion plays a crucial role in determining the extent of excision required.
- If the lesion measures less than 1 mm in depth, a 1 cm diameter margin is typically excised from the surrounding area of the lesion
- If the lesion measures 1 mm to less than 2 mm in depth, a 2 cm diameter margin is typically excised from the surrounding area of the lesion
- If the lesion measures greater than 2.01 mm in depth, a 2 cm diameter margin is generally excised from the surrounding area of the lesion
Depending on the specific circumstances, your surgeon may recommend additional procedures such as a sentinel lymph node biopsy (SNLB) or a regional lymph node biopsy to assess whether the melanoma has spread beyond the immediate area. Further treatment options, such as immunotherapy, chemotherapy, or radiation therapy, may be considered based on the stage of the melanoma.
What happens after the excision?
After the lesion is surgically excised and the wound is closed using either permanent or dissolving sutures, it is sent to a pathologist for microscopic examination. This examination is conducted to confirm the diagnosis and determine the depth of the lesion.
Following your surgery, there will be a follow-up appointment at the office or clinic after approximately 5-7 days for facial lesions or 10-14 days for lesions on other parts of the body. During this visit, you will review the pathology report, assess the condition of your incision, and have any necessary sutures removed or trimmed. At this time, the healthcare professional will discuss the need for further local excision or the possibility of systemic management. If necessary, you will be referred to the appropriate specialist for further evaluation and treatment.

What can I do to prevent melanoma?
Following a diagnosis of melanoma and completion of all necessary treatments, it is important to maintain regular follow-up appointments to monitor the area where the lesion was located for any potential signs of recurrence. Additionally, scheduling yearly skin examinations is highly recommended to detect any new lesions at an early stage, facilitating prompt treatment.
Protecting the skin from further sun damage remains crucial. It is advised to wear hats and clothing that provide coverage for exposed skin, along with the consistent use of sunblock. These preventive measures are essential in preventing the development of additional skin cancers.