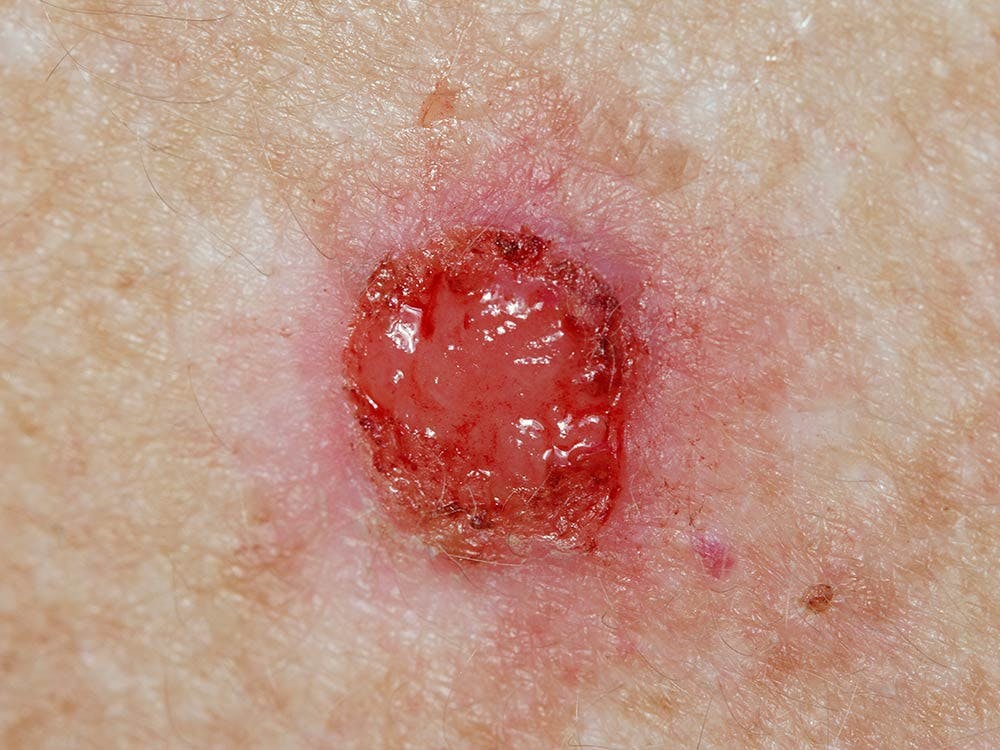
What is Basal cell carcinoma (BCC)?
Basal cell carcinoma is the most common type of skin cancer that arises from the basal layers of the skin and typically shows up in sun-exposed areas such as the head, neck, trunk and extremities.
Schedule a complimentary consultation today!
ScheduleIs basal cell carcinoma dangerous?
Although basal cell carcinomas (BCCs) are fairly indolent lesions, they are locally growing and can be locally invasive. This means that the growth can get larger over time and invade into deeper and surrounding tissues of the body, such as tendons, nerves and bones.
Metastasis (cancer spreading to a distant part of the body), however, is extremely rare.
What causes basal cell carcinoma?
Basal cell carcinoma is often more prevalent in individuals with lighter skin and is caused by cumulative sun exposure.
Other established risk factors include UV tanning beds, chronic arsenic exposure, previous radiation therapy and immunosuppressant medications for other conditions.

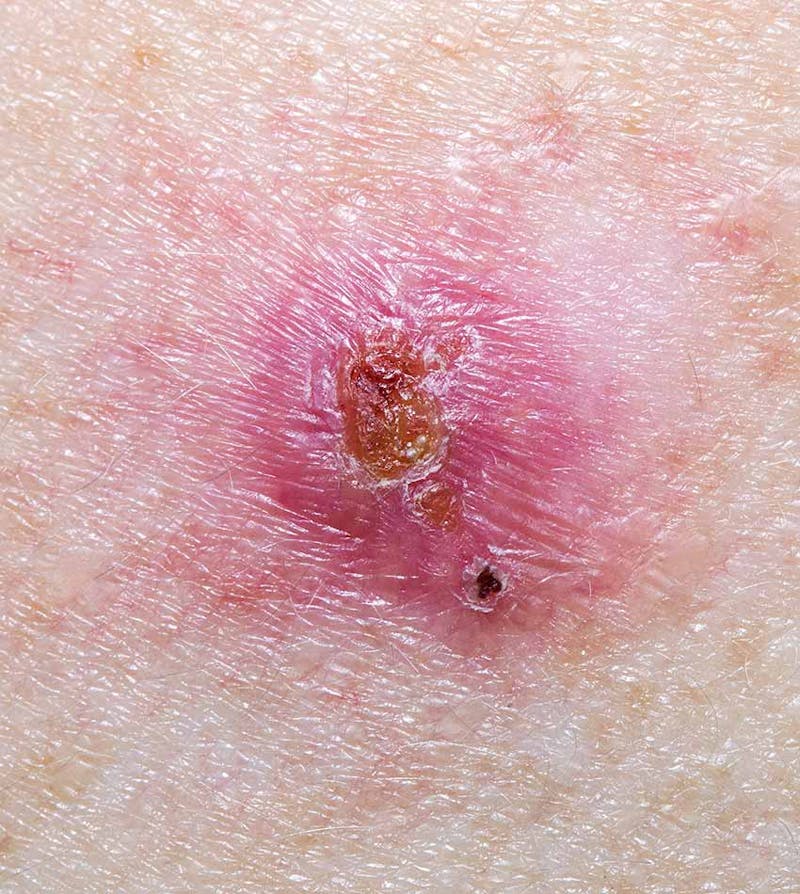
What do the basal cell carcinoma lesions look like?
70% of BCCs develop on the face, about 15% present on the trunk, and very rarely BCCs can be found in genital areas.
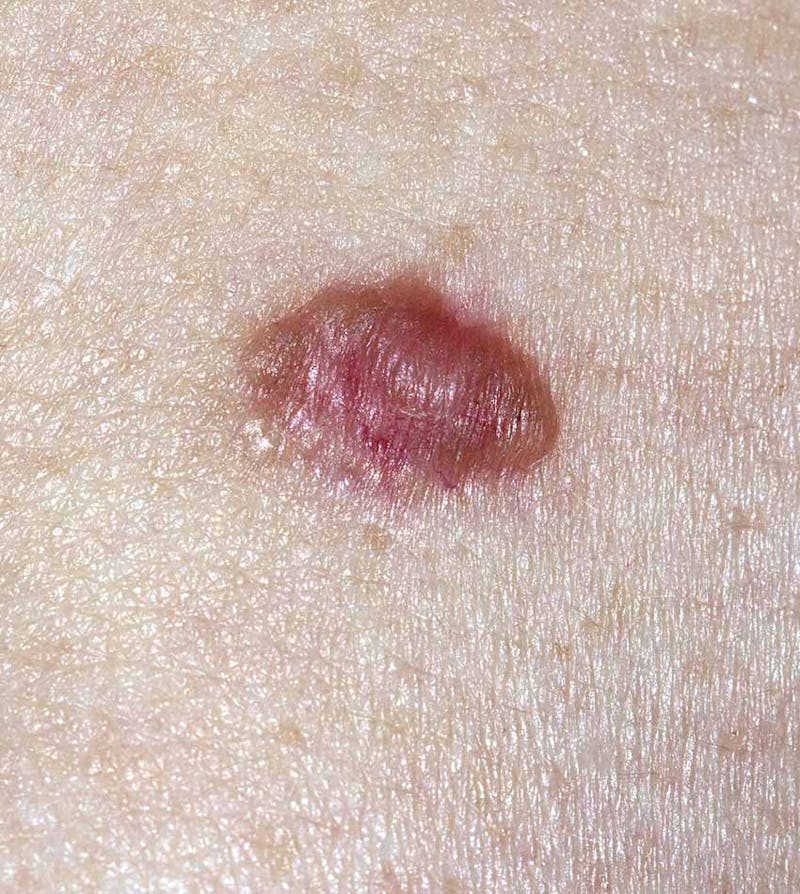
BCCs look like flesh-coloured papules that have a pearly/translucent quality. You may see some tiny blood vessels that run through the lesions. They may have a raised or rolled border with a depressed center or an ulcerated middle.
What are my treatment options?
There are different ways of treating BCC. If the lesion is small and caught early, the lesions can be frozen (with cryotherapy) or burnt off (with electrocautery) which causes minimal scaring. There are prescription creams, such as imiquimod and topical 5-FU that can be used in superficially spreading BCCs.
Complete excision for larger lesions or lesions in visible areas can help achieve the best medical and aesthetic results.

What happens after my procedure?
Once the lesion is removed and the wound is sealed using either permanent or dissolving sutures, it is forwarded to a pathologist for microscopic examination. This step is crucial to verify the diagnosis and ensure that the entire lesion has been successfully excised.
Following the surgery, there is a wait of approximately 5-7 days for facial lesions or 10-14 days for lesions located on other parts of the body. During this period, you will return to the office or clinic for a follow-up appointment. The purpose of this visit is to go over the pathology report, assess the condition of your incision, and either remove or trim your sutures as necessary.

What can I do to prevent basal cell carcinomas?
If you have skin cancers removed and have risk factors for development of BCCs, you should schedule yearly skin examinations to ensure that you catch these lesions early and have them treated in a timely manner.
Additionally, protection from sun damage is important. The use of hats and clothing that cover exposed skin as well as sunblock is vital to prevent the development of more skin cancers.